UV light reveals COVID-19 exposure due to improper PPE use
por
John R. Fischer, Senior Reporter | May 11, 2020
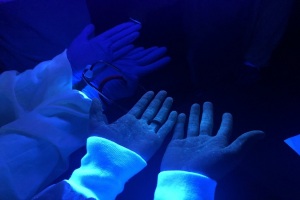
Ultraviolet light can visually depict how aerosol-generating procedures can expose healthcare workers who are improperly using PPE to COVID-19.
A new technique employing a nontoxic fluorescent solution and ultraviolet light can reveal who among healthcare workers has been exposed to COVID-19 due to improper use of personal protective equipment (PPE).
Dr. Patrick G. Hughes, D.O., of Florida Atlantic University’s Schmidt College of Medicine and collaborators at the University of Arizona College of Medicine – Tucson and the Indiana University School of Medicine developed and used the approach during a training session to visually show how aerosol-generating procedures can expose healthcare workers who have not put on or taken off PPE correctly to the virus.
“This training method allows educators and learners to easily visualize any contamination on themselves after they fully remove their personal protective equipment,” said Hughes, the lead author, director of FAU’s emergency medicine simulation program and an assistant professor of integrated medical science at FAU’s Schmidt College of Medicine, in a statement. “We can make immediate corrections to each individual’s technique based on visual evidence of the exposure.”
Submerging a highlighter refill in a warm water bath for 15 minutes, the team produced the fluorescent solution, which can only be seen under ultraviolet light. It applied the solution to a simulated albuterol nebulizer treatment, used to represent the contagion.
The researchers then instructed a group of healthcare staff members to don caps, gowns, surgical gloves, eye protection, face shields and N95 masks, and go into a non-negative pressure room to care for a simulated patient, all of which were sprayed down with the invisible simulated contagion. The group was then taken to another room where the lights were turned off. There, the ultraviolet light revealed widespread simulated contagion on gloves and gowns from directly touching the simulated patient, and on face shields and masks from the aerosolized solution.
The team used a black light flashlight to examine each worker and identify the presence of any fluorescent solution, before allowing them to completely remove their PPE. They found the fluorescent solution on the skin of healthcare workers that did not follow PPE guidelines, validating exposure to the contagion due to improperly putting on or taking off PPE. The most common error made was contamination of the face or forearms during PPE removal. Those who did follow guidelines, however, showed no signs of the fluorescent contagion on their skin or face.
“This experiment demonstrated that following PPE training improves workplace safety and decreases the risk of transmission,” said Hughes. “This simulation-based approach provides an efficient, low-cost solution that can be implemented in any hospital.”
Study co-authors are Kate E. Hughes, D.O., emergency medicine, University of Arizona College of Medicine – Tucson; and Rami A. Ahmed, D.O., emergency medicine, Indiana University School of Medicine, Indianapolis.
The findings were published in the journal, Medical Education.
|
|
|
You Must Be Logged In To Post A Comment
|
